What to Expect with a Corneal Transplant

Receiving a keratoplasty is often the best way to improve eyesight for patients whose corneas have been irreparably damaged.
Keratoplasty, also known as corneal transplant surgery, is a relatively common operation that’s performed tens of thousands of times in the United States every year. Patients who receive a corneal transplant can expect benefits including better vision, reduced pain, and the improved appearance of their damaged cornea.
While the procedure is successful the vast majority of the time, patients should always be fully informed before undergoing a corneal transplant. Below, we explore the most important things for potential corneal transplant recipients to know about the procedure.
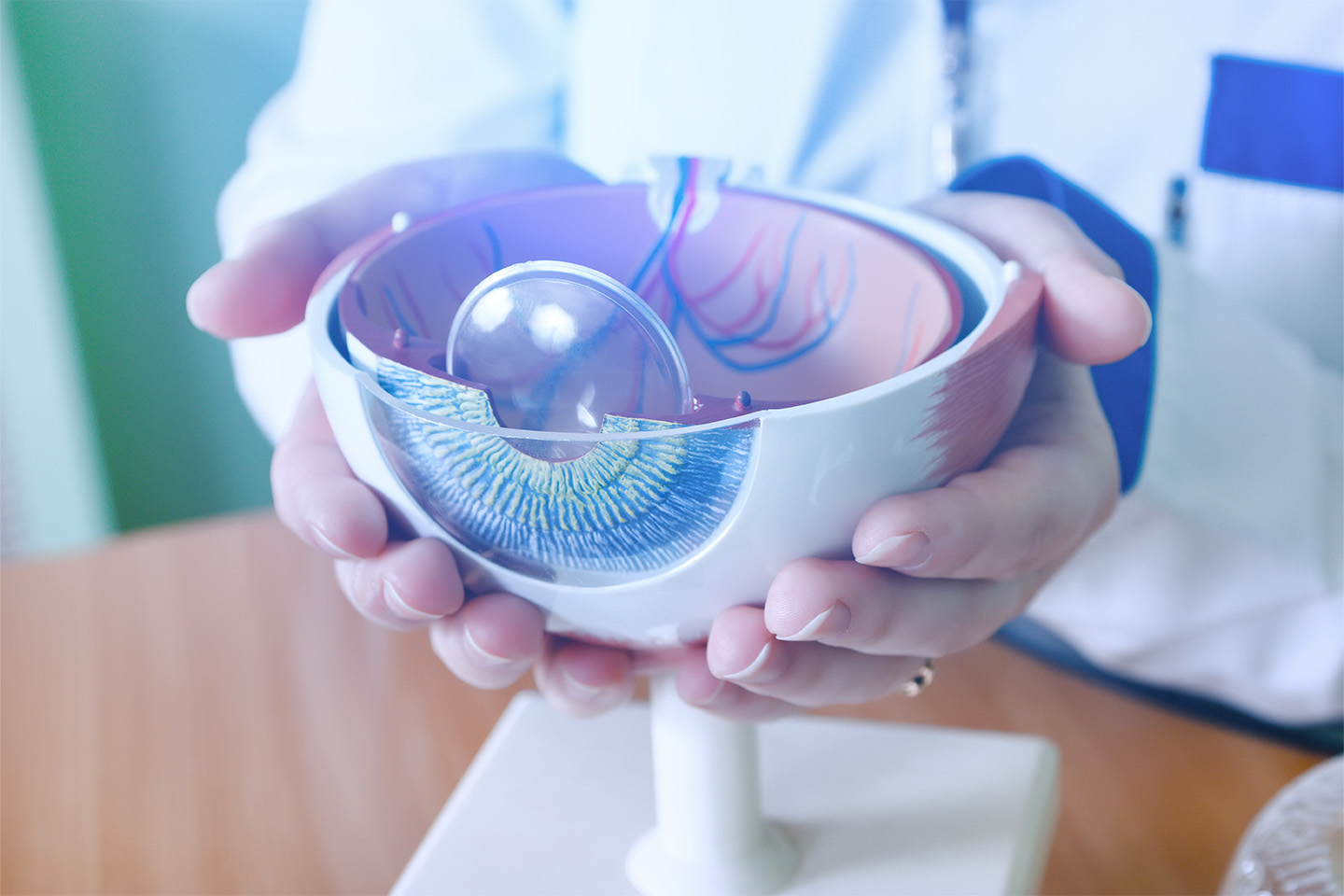
What Is a Corneal Transplant?
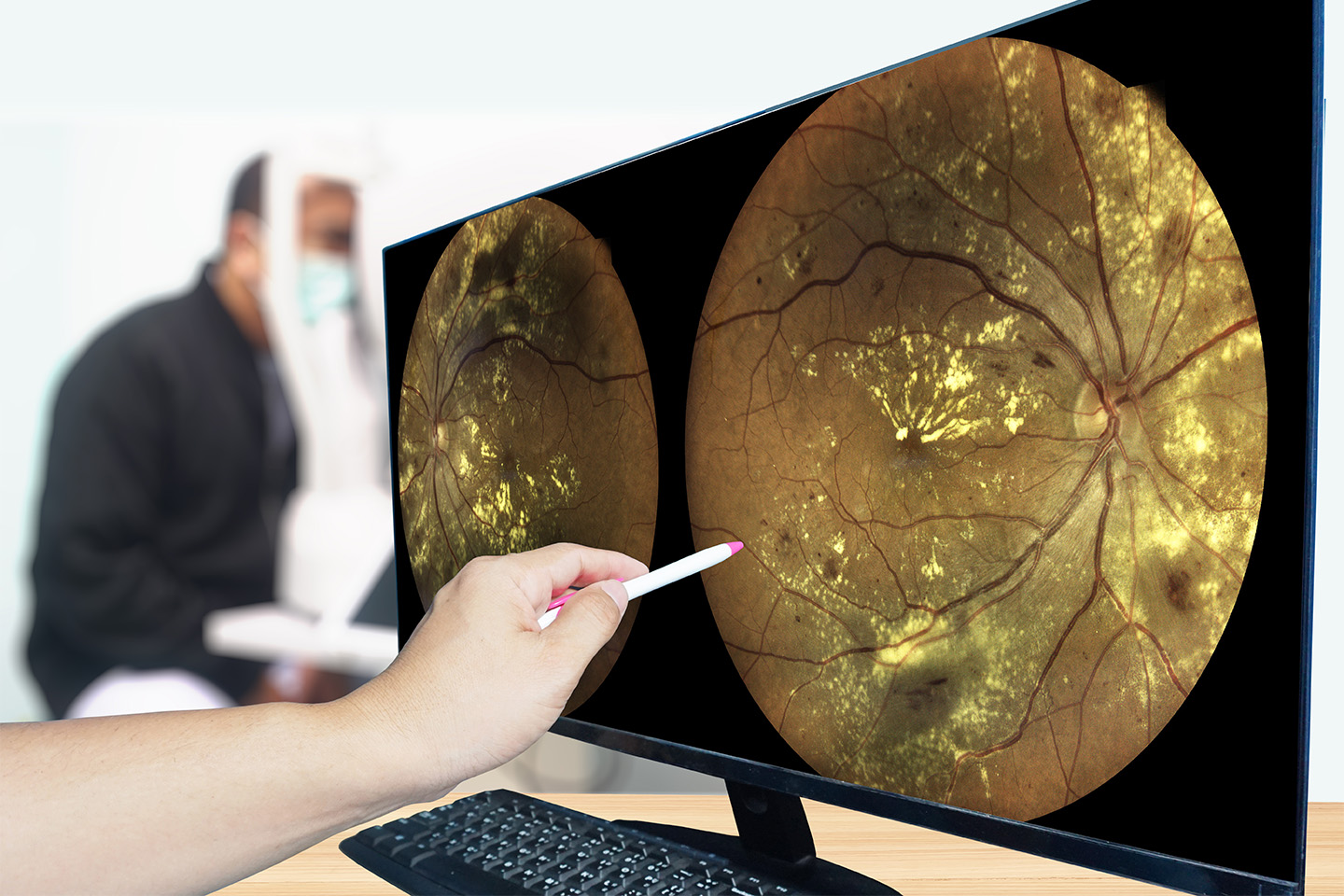
The cornea is the transparent, dome-shaped surface of the eye. It’s responsible for helping the eye focus, and serves as the “protective window” that allows light to enter the eye. Unhealthy corneas will cause glare, blurred vision, and scattered light.
When a cornea becomes damaged or diseased, a corneal transplant may become necessary. There are several common reasons why a patient may need a corneal transplant, including corneal scarring caused by eye infections or injuries, Fuchs’ dystrophy, and keratoconus, a condition in which the cornea is shaped like a cone rather than a dome.
There are two main types of corneal transplants: keratoplasty, which is a traditional, full-thickness corneal transplant, and endothelial keratoplasty. The latter type targets the back layer of the cornea. In both instances, a graft replaces a portion of the patient’s corneal tissue with healthy tissue that has been donated to a local eye bank.
The best candidates for a corneal transplant have impaired vision that impacts their ability to perform daily tasks and cannot be corrected by eyeglasses or contact lenses. Here’s what these patients can expect from a corneal transplant procedure.
The Corneal Transplant Procedure
Patients interested in receiving a corneal transplant must first talk to their ophthalmologist about the procedure and be sure to notify them about any medications they’re taking — doctors usually recommend that patients stop taking blood thinners for a short period of time before they receive a keratoplasty. Prior to surgery, your ophthalmologist will give you a comprehensive eye exam during which they will carefully measure your cornea, ensuring the donated cornea is sized correctly.
During the procedure, a patient is given medicated eye drops as well as either a local or general anesthetic (depending on the patient’s health, age, and personal preference). Once the anesthesia kicks in, the surgeon will cut through the thickness of the cornea using an instrument called a trephine or a femtosecond laser and remove a small disk of corneal tissue. In the most common form of corneal transplant surgery (keratoplasty), most of the corneal tissue is removed, however there are other variations of the procedure in which only specific layers are replaced.
After the damaged or infected tissue is removed, the donor cornea will be inserted into the opening. Then, the surgeon will use a fine thread to stitch the cornea back together. Once the sutures are complete, the surgeon will cover your eye with a shield to keep it safe. The stitches may be left in your eye for up to a year after the surgery.
While a corneal transplant is an outpatient procedure, patients are not allowed to drive themselves home from the surgery. As such, you will need to make plans to have someone else transport you on the day of your transplant.
What to Expect After a Corneal Transplant
While most patients can return to their normal routine within a day or two of receiving a corneal transplant, and can expect their vision to stabilize within a few weeks, it can take six months to a year for the eye to fully recover. In the days, weeks, and months following a corneal transplant, patients will need to regularly visit their ophthalmologist for follow-up appointments.
In the immediate aftermath of a corneal transplant, patients are advised to use eye drops and take pain medication as prescribed. The eye will also need to stay covered for a period of time, and patients should not rub or press on their eye. It’s not unusual for your vision to be worse than before your surgery at first, as your eye will need time to adjust to its new cornea. However, once your cornea has healed (usually within several weeks), you can expect to have considerably better vision than you had before.
As with any surgery, a corneal transplant comes with some risk. In about 10 percent of cases, a patient’s body will reject the transplanted cornea. This issue can be resolved either with prescription medication or a second corneal transplant procedure. If you’ve received a corneal transplant and are experiencing eye pain, sensitivity to light, eye redness, or cloudy vision, check with your ophthalmologist to make sure there are no problems with the transplant.
If you believe you might need a corneal transplant, consider reaching out to the eyecare experts at the Kleiman Evangelista Eye Centers of Texas. Our experienced team can help you determine whether a corneal transplant procedure would be right for you. If you’d like to get the conversation started, schedule a consultation today.
Turn To The Top Eye Doctors In Texas
Check out one of our locations below for the best eye care near you:
[DISPLAY_ULTIMATE_SOCIAL_ICONS]