Glaucoma often develops slowly and without noticeable symptoms. That’s why regular eye exams and early intervention are critical. Here’s what your glaucoma journey may look like:
Concerned about your eye pressure or glaucoma diagnosis? Schedule an appointment to talk with your eye care provider today!
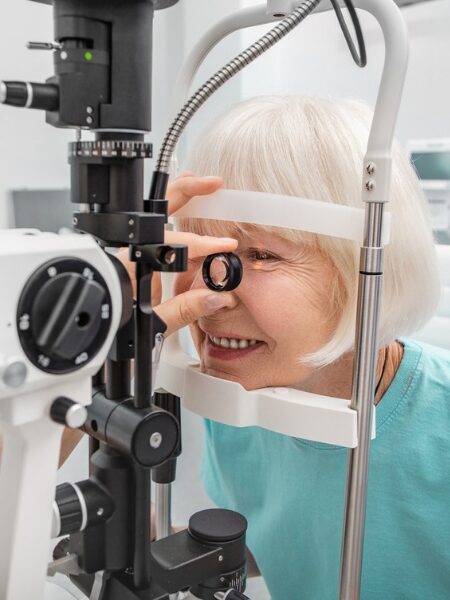
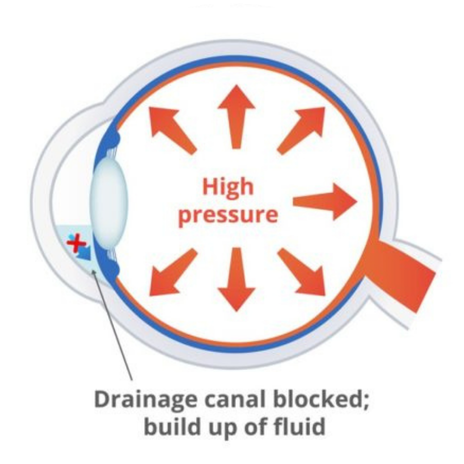
Glaucoma is caused by damage to the optic nerve, often due to pressure building up inside the eye. That pressure typically comes from fluid that can’t drain properly. Over time, high pressure can damage the nerve and lead to vision loss, especially peripheral vision.
We tailor your care based on your type of glaucoma, lifestyle, and overall eye health. Our goal is to reduce eye pressure, slow disease progression, and preserve vision, with minimal disruption to your life.
Prescription eye drops that reduce pressure by either helping fluid drain better or lowering fluid production in the eye.
Performed on their own or at the time of cataract surgery, MIGS procedures offer long-term pressure control with minimal recovery.
For more advanced cases:

Dr Glanzer was very knowledgeable and explained everything in easy to understand terms. Made a plan to try to resolve the problem I’m having with my vision
My experience was great. We talked about my vision as a relates to lifestyle and chose a plan that would suit my lifestyle....which made me feel really comfortable with the plan that we chose.
Thank you for taking the time to explain your approach for monitoring my condition and options available to me.
Typically performed with cataract surgery, these innovative treatments are now available independently for patients with or without a cataract diagnosis. Offering these as standalone procedures enhances accessibility and convenience for advanced glaucoma care.
To explore your glaucoma treatment options, contact Kleiman Evangelista Eye Centers today to schedule a consultation.
Please check with your insurance provider to see if these procedures are covered.
If you’ve been diagnosed with glaucoma or elevated eye pressure, it’s important to work with your eye doctor to monitor your condition. If drops alone aren’t working, you’re having trouble with side effects, or are looking for treatment options that reduce dependency on drops, ask about additional treatment options like laser treatment or MIGS procedures.
While glaucoma can’t be cured, it can be managed. Our goal is to protect your vision by lowering eye pressure and slowing disease progression with the right combination of treatments.
MIGS stands for minimally invasive glaucoma surgery. These procedures can be done at the same time as cataract surgery or as standalone options. They offer faster recovery and fewer risks than traditional surgeries while still effectively lowering eye pressure.
Some patients are able to reduce or eliminate their reliance on eye drops, but it depends on the severity of your condition. We’ll personalize your treatment plan to help you achieve the best possible pressure control with the fewest medications.
Yes. Most glaucoma procedures, including SLT, MIGS procedures, and traditional surgeries, are covered by insurance, including Medicare. Our team can help you understand your coverage.