Is it Possible to Stop the Progression of Keratoconus?

Although doctors are still researching the cause of keratoconus, there are plenty of treatments to help manage symptoms and slow its progression.
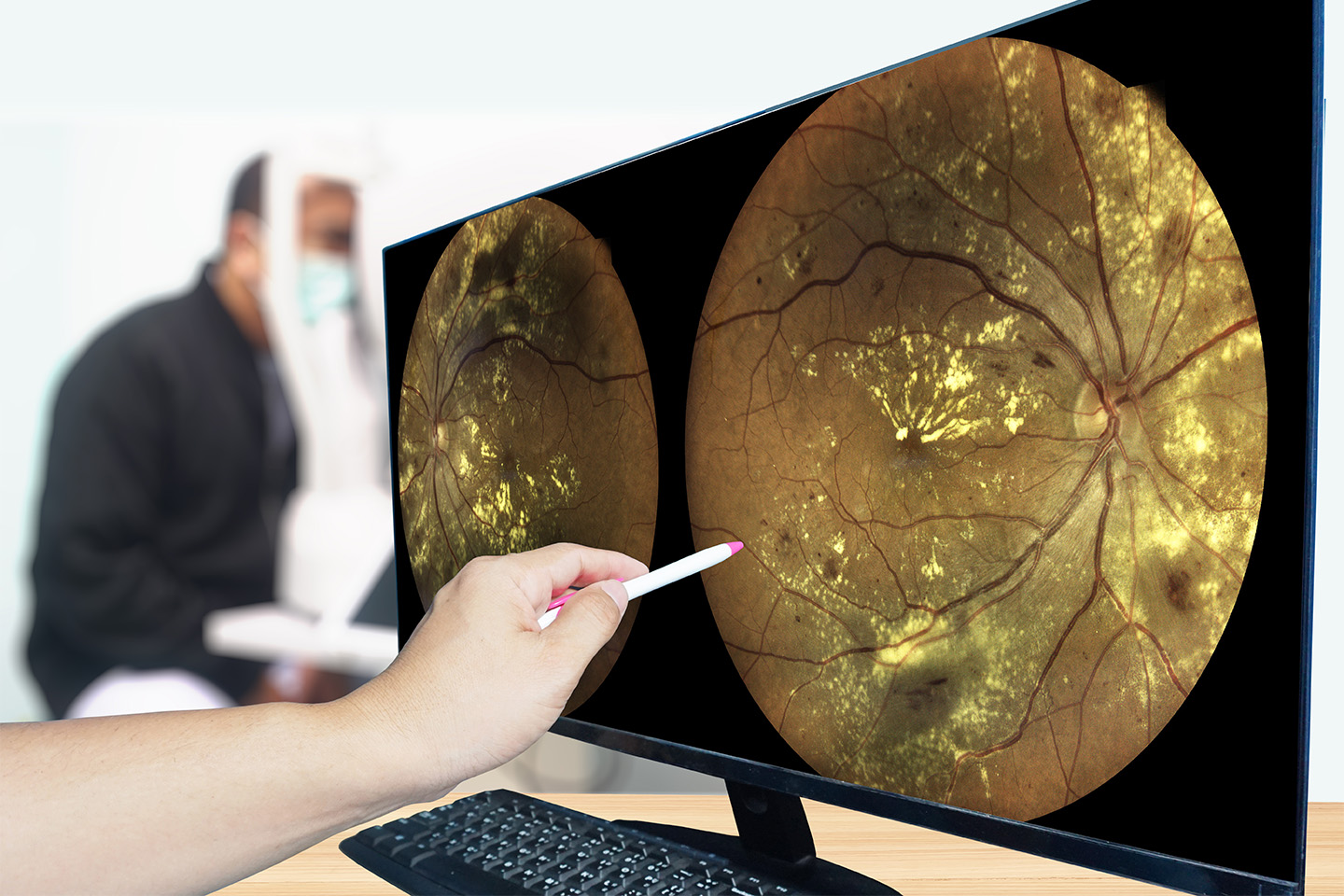
Keratoconus — sometimes referred to as conical cornea — is a progressive eye disease that causes a person’s cornea to thin and bulge into a cone-shape. Typically, keratoconus affects one in every 2,000 individuals, although a recent study from The American Journal of Ophthalmology argues that cases may be as high as one in every 375 individuals.
A typical, healthy cornea has a dome-like shape which is held together with tiny fibers of protein called collagen. This round shape allows the cornea to properly control the entry of light into the eye to help us see.
Patients with keratoconus, however, have weaker collagen. As a result, their cornea progressively become thinner and cone-shaped. Keratoconus often starts in one eye before eventually progressing to both. These changes might happen quickly, or develop over several years.
When the cornea becomes conical, it has trouble properly conveying images to the brain. This often causes blurred or distorted vision, astigmatism, double vision, inability to see in dim light, nearsightedness, and sensitivity to light.
What Causes Keratoconus?
Unfortunately, doctors are not yet certain as to what causes keratoconus. Many believe the condition is genetic, as roughly 10 percent of keratoconus patients also have a parent living with the condition. In other cases, keratoconus symptoms are associated with allergies and excessive eye rubbing. Likewise, some believe exposure to ultraviolet light might increase the risk of keratoconus.
Although researchers have not yet identified a definitive cause, The National Eye Institute recently gave a $2.1 million grant to the Medical College of Georgia to enable doctors to pursue research into the causes of keratoconus. Because a previous link between a mutation in the PPIP5K2 gene and the onset of keratoconus has been established by doctors, this grant money is being used to further investigate the genetic component of the disease.
Treatments for Keratoconus
Although doctors are still searching to understand what causes keratoconus, patients can still explore several options to lessen their symptoms and improve their vision.
For mild cases of keratoconus, simply purchasing eyeglasses or soft contact lenses can help patients get relief from their symptoms. But as the disease progresses and the cornea continues to thin, patients may need to take more serious action.
For more moderate cases of keratoconus, patients can undergo corneal-cross linking. This procedure — which may also be referred to as CXL — aims to strengthen corneal tissue to stop the bulging of the cornea in keratoconus. The two primary methods of CXL are epithelium-off and epithelium-on.
Epithelium-off is the process of removing the outer layer of the cornea (called the epithelium) so doctors can administer riboflavin eye drops directly into the eyes. Then, a UV light is directed over the cornea, which causes a reaction in collagen fibers inside the cornea. This will strengthen the cornea to stop it from bulging.
Epithelium-on is a similar method, but the corneal epithelium is left intact during the treatment. Instead, doctors simply administer a higher volume of riboflavin to penetrate the cornea. Although this may be less effective, it is a more comfortable procedure with almost no risk of infection and a faster recovery time.
If eyeglasses, contact lenses, and other treatments fail to improve a patient’s symptoms, the next best option may be a corneal transplant. This requires replacing the center of the cornea with a donor cornea. This should only be considered in severe cases.
The Road to Clearer Vision
Although doctors don’t know with certainty if keratoconus is preventable or what it causes it 100 percent of the time, they do know that its effects can be prevented with the right options. At Kleiman Evangelista Eye Centers of Texas, our doctors can diagnosis keratoconus with a thorough eye exam and walk you through treatment options that you’re comfortable with.
If you think you may have keratoconus or another eye condition, don’t hesitate to make an appointment with us today.
Turn To The Top Eye Doctors In Texas
Check out one of our locations below for the best eye care near you:
[DISPLAY_ULTIMATE_SOCIAL_ICONS]